Op-Ed: America’s Healthcare System can’t Handle a Pandemic
January 13, 2021
America can’t catch a break with COVID-19.
If people avoid being laid-off, then they could get sick at work. If people do get laid off, then they lose their health insurance, adding pressure onto COVID-19 victims. Thus, the pandemic reveals holes in American health insurance that weren’t obvious before.
The issue is that while the unemployed have insurance options, these options are disjointed. This results in coverage gaps – either people are uninsured for periods of time, or there are segments of the population who lack coverage.
These problems could be addressed through a universal healthcare system. But first, let’s examine the issues with America’s current system.
Healthcare is tied to Employment — Bad Idea
In March 2019, 69% of American workers had employer-based insurance. If you lose your job, you lose insurance.
This was exacerbated in 2020, as the country experienced a recession with over a million jobless claims each week.
Between 3.5-27 million have lost insurance this year, according to estimates from the Urban Institute, Families USA, and Kaiser Family Foundation (KFF). The 27-million estimate considers dependents who lose coverage (e.g. children).
This data implies that the US has an insurance crisis – it’s possible that people may be less likely to get treatment if they’re sick. If they do get help, then they’ll struggle with medical bills.
Finding Alternate Insurance
Unemployed individuals have 3 primary coverage options, COBRA, Obamacare, and Medicaid. Let’s discuss each.
COBRA (Consolidated Omnibus Budget Reconciliation Act)
The first option for unemployed people is COBRA. It lets someone continue to receive coverage through their employer after losing their job.
Here’s the gist: if you lose your job (or are forced to work part-time), then you can register for COBRA within 60 days. You’ll get the same coverage that you had for 18–36 months. However, you have to pay much more.
Normally, your employer pays most of your health insurance premiums (the periodic fees that your insurance company takes). For example, your employer pays 80% and you pay 20%. However, if you enroll in COBRA, you take on all of the premiums.
The idea is to have an organized system to help people continue coverage after losing their job. They don’t have to find a job immediately to get insurance, as COBRA is available (for companies with 20+ employees). But businesses won’t pay insurance after you leave, so you take on the burden.
It’s not ideal, and having your bills spike during a pandemic is problematic.
But COBRA is only meant to be a brief transition state, not a long-term solution for the unemployed. So what’s the next option?
Obamacare Marketplaces
The Affordable Care Act (ACA, also known as Obamacare) established an insurance marketplace known as healthcare.gov. Here, there are tons of private insurance plans. If someone is in between jobs, then they can enroll to find a plan. Obamacare also did the following:
- Subsidized insurance-plan costs.
- Reimbursed insurance companies who had to offer cheaper healthcare.gov plans.
- Implemented outreach to help people sign up.
This goal was to slash prices through greater competition on the healthcare.gov exchange. It also gave people a quick(er) way to find insurance while in-between jobs.
Unfortunately, the Trump administration cut company’s reimbursements and outreach funding. Now, insurance companies can push back against providing cheaper plans, making it harder for people to sign up with healthcare.gov.
There’s one more option…
Medicaid
If you lose your job and struggle financially, you can qualify for Medicaid. However, enrollment takes 45–90 days. That’s a giant window where you’re left uncovered.
Another issue is that — with millions losing insurance — we could see a wave of enrollment in Medicaid. KFF estimated that 17 million people could be eligible for Medicaid by January 2021. Medicaid could become more overburdened with sick people if COVID-19 gets worse.
Also, KFF estimated that 6 million people could become eligible for Obamacare subsidies. It projected a “coverage gap” of 1.9 million Americans – these are people who make too much to qualify for Medicaid, but not enough to qualify for Obamacare.
COVERAGE GAPS
One part of Obamacare was “Medicaid expansion.” Many states expanded Medicaid by increasing the financial threshold to qualify — people with slightly higher incomes can qualify now in many states. With that, the Obamacare subsidies are only offered to people above the Medicaid threshold.
However, some states didn’t expand Medicaid: they’re still at the lower threshold. In these states, there’s a gap between the Medicaid upper threshold and the Obamacare lower-threshold. This gap could leave 1.9 million uninsured.
Too Many Holes — We Need Universal Healthcare
People lose their insurance if they get fired due to the recession, but they need insurance because we have a pandemic.
As I have outlined, Americans can then get COBRA (which is pricey), ACA marketplace (which Trump undermined), or Medicaid (which will leave them uncovered for weeks).
The problem is that our system is fragmented. We have many programs with separate qualifications that don’t align, making transitions cumbersome. If people can’t access one system, then they’ll flock to another and overburden it.
A universal system that covered everyone could address these issues.
If everyone used one mechanism, then people would always be covered, costs would be constant, and people wouldn’t worry about switching between programs. The risk would also be spread evenly over everybody.
During a pandemic, people can’t waste time figuring out insurance. People should have coverage when they need it — that helps accelerate treatment and fight the virus. Having a single, universal system can help.
For example, in Canada, Australia, and European countries, the government covers everyone. All residents are automatically enrolled, and tax dollars constantly fund insurance so that people don’t think about enrollment. This is known as a “single-payer” system (the government being the ‘single-insurer’).
Alternatively, countries like Switzerland also have universal healthcare, but they do it by regulating private insurance. People are mandated to buy insurance, private insurers are required to cover needs, and insurance costs are subsidized. People can buy insurance from whichever insurance provider that they want (increasing competition and decreasing prices), unlike here where your employer dictates your provider.
The negative effects of the US healthcare system are evident. As of April (admittedly early), 33% of Americans skipped care due to costs – higher than other countries. That could be because countries with universal healthcare have mechanisms built in to reduce costs more so than America. A universal system could bring down costs and make the crisis easier to manage for the government and for individuals.
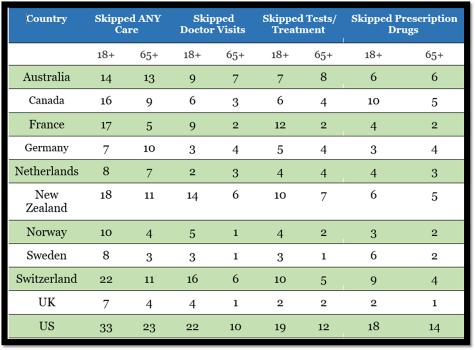
Percentage of individuals who skipped care for various reasons by country. 33% of Americans “skipped ANY care” as opposed to 22% of Swiss people and between 7-18% of people in other countries. The US is considerably higher than other countries in all 4 categories – both for adults above 18 and for seniors above 65. Source: Commonwealth Fund.
The point is that – while no system is perfect – there are government-based and market-based ways to reach universal coverage. We’re not discussing this enough. A universal system, whatever it looks like, would help manage COVID-19 in an orderly way, unlike our (relatively) disorganized approach.
People are encountering problems due to COVID-19 that are not immediately obvious. Let’s not forget that.








